 
This gives the short PR interval and slurred upstroke to the QRS complex known as the delta wave. Since the accessory pathway does not have the impulse slowing properties of the AV node, the electrical impulse first activates the ventricles via the accessory pathway, and immediately afterwards via the AV node. In individuals with WPW syndrome, electrical activity that is initiated in the SA node travels through the accessory pathway as well as through the AV node to activate the ventricles via both pathways. When an individual is in normal sinus rhythm, the ECG characteristics of WPW syndrome are a short PR interval, widened QRS complex (greater than 120ms in length) with slurred upstroke of the QRS complex, and secondary repolarization changes reflected in ST segment-T wave changes. This combination of atrial fibrillation and WPW is considered dangerous, and most antiarrhythmic drugs are contraindicated. If the patient experiences episodes of atrial fibrillation, the ECG will show a rapid polymorphic wide-complex tachycardia (without turning of the points-also known as torsades des pointes). The short PR interval and slurring of the QRS complex is actually the impulse making it through to the ventricles prematurely (across the accessory pathway) without the usual delay experienced in the AV node. In this case it is manifested as a delta wave, which is a slurred upstroke in the QRS complex that is associated with a short PR interval. WPW syndrome is commonly diagnosed on the basis of the surface ECG in an asymptomatic individual. In some cases, the combination of an accessory pathway and cardiac arrhythmias can trigger ventricular fibrillation, a leading cause of sudden cardiac death. Extremely fast heart rates are potentially dangerous, and can cause hemodynamic instability. For instance, in the example above, if an individual had an atrial rate of 300 beats per minute, the accessory bundle may conduct all the electrical impulses from the atria to the ventricles, causing the ventricles to activate at 300 beats per minute. 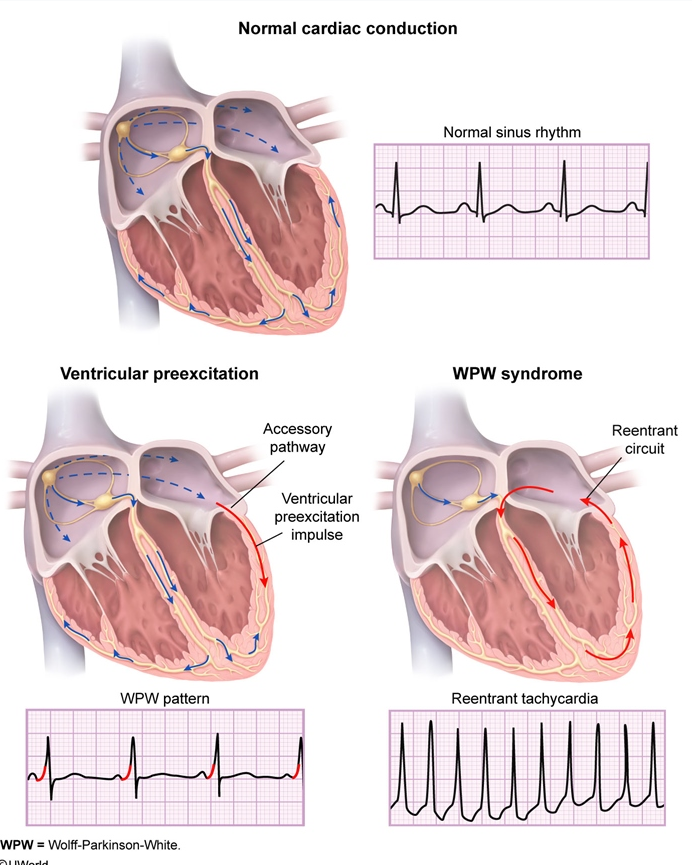
This accessory pathway does not share the rate-slowing properties of the AV node, and may conduct electrical activity at a significantly higher rate than the AV node. This accessory pathway is known as the bundle of Kent. Individuals with WPW syndrome have an accessory pathway that connects the atria and the ventricles, in addition to the AV node. This is manifest on the ECG as the PR interval, the time from activation of the atria (manifest as the P wave) and activation of the ventricles (manifest as the QRS complex). Another important property of the AV node is that it slows down individual electrical impulses. For instance, if the atria are electrically activated at 300 beats per minute, half those electrical impulses are blocked by the AV node, so that the ventricles are activated at 150 beats per minute (giving a pulse of 150 beats per minute). This function of the AV node is important, because if the signals generated in the atria of the heart were to increase in rate (as they do during atrial fibrillation or atrial flutter), the AV node will limit the electrical activity that conducts to the ventricles. 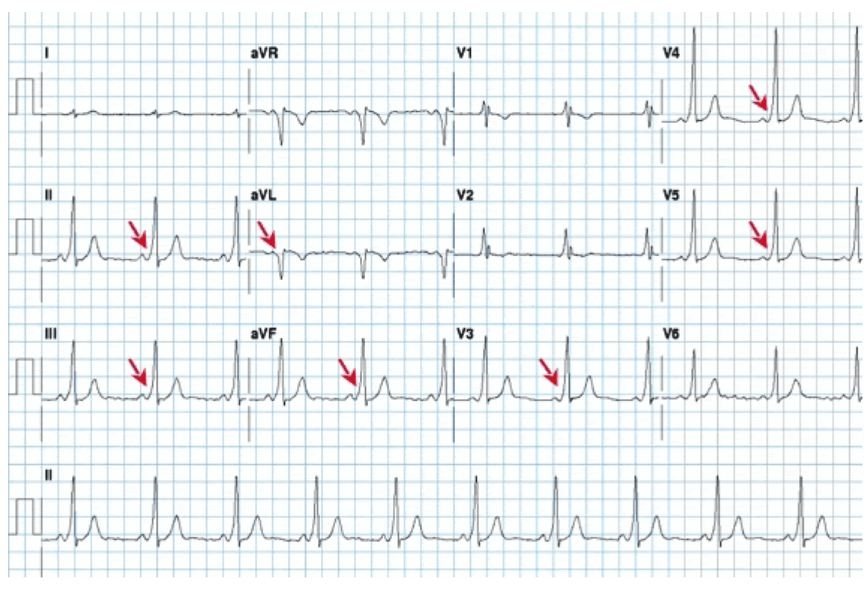
The AV node acts as a gatekeeper, limiting the electrical activity that reaches the ventricles of the heart. (See electrical conduction system of the heart). In normal individuals, electrical activity in the heart is initiated in the sinoatrial (SA) node (located in the right atrium), propagates to the atrioventricular (AV) node, and then through the bundle of His to the ventricles of the heart. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
